Trigger Point Dry Needling
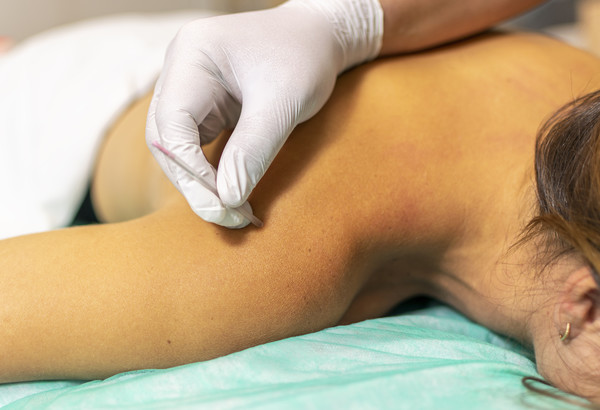

Trigger point dry needling technique uses a solid filament needle to treat muscle trigger points which are causing pain and discomfort. A trigger point is a hyperirritable taut band of skeletal muscle fibers within a muscle. Myofascial trigger points can play a role in producing pain. A physical therapist trained in the use of dry needling will insert the needle through the skin stimulating myofascial trigger points and muscular and connective tissues. The goal is to release or inactivate the trigger points to help relieve pain or improve range of motion.
What is the treatment?
Dry needling is used to treat myofascial pain syndrome. This is a regional muscular pain condition. Myofascial pain syndrome has been recognized by medical practitioners as contributing or causing sensory, motor, and autonomic impairments. It is normally associated with palpable muscle “knots” or taut bands known as myofascial trigger points, which can be addressed with dry needling.
A trigger point is defined as a focal, hyperirritable nodule located in a band of skeletal muscle that results in local or referred pain with mechanical stimulation. Trigger points are palpable knots most commonly found in the center of a muscle belly. Any skeletal muscle in the body is susceptible to develop trigger points, which can be caused by acute trauma, or repetitive muscular stress. Trigger points are also often linked with chronic musculoskeletal disorders. Symptoms can include local/referred pain, increased sensitivity, muscle spasm, muscle stiffness, muscle weakness, decreased range of motion, and autonomic dysfunction. Common causes of trigger points are:
- Acute trauma
- Chronic stress conditions (anxiety, depression, psychological stress)
- Dietary deficiencies
- Lack of exercise
- Muscle overuse/overtraining
- Repetitive muscular stress
How is it performed?
A solid monofilament needle is inserted directly through the skin and muscle into an active or latent trigger point. No chemical agents are used. The mechanical stimulation created by the needle elicits a twitch response, causing the tissue to disengage and “release”. Enabling the trigger point to deactivate in the dysfunctional muscle will often result in reduced symptoms and improved mobility.
Number of treatments depends on the primary condition being treated and the tissue involved. Effectiveness is measured by how your body shows improvement in your functional movements, and not by pain reduction alone. Effects of dry needling remain for up to four weeks after the intervention. However, to meaningfully reduce a patient’s pain long-term requires sustained improvement in the patient’s functional movements through a comprehensive treatment plan to include manual therapy, targeted exercises, neuromuscular re-education, and addressing biomechanical dysfunctions.
It is common and expected to have soreness in the tissue that was needled to last 24-48 hours. It should dissipate each day.
Following dry needling treatments, in order to attain the most benefit, the patient should:
- Promote circulation in the muscle/tissue that was needled.
- Keep moving! Frequently and repetitively move the part of the body that was needled.
- Avoid prolonged postures or sedentary positions.
- Use heat.
- Avoid ice. This causes restricted circulation.
- Stay hydrated.
- Drink lots of water for better cellular circulation.
- Limit diuretic drinks such as caffeine and alcohol.
- Light stretching is encouraged.
What are the benefits?
Dry needling is a low risk, inexpensive intervention, and can only be performed by physical therapists who are certified by their state board. Dr. Janet Travell and Dr. David Simons pioneered the treatment in the 1940s by their discovery that injections of analgesic medication into trigger points caused a decrease in symptoms, pain, and sensitivity to touch. Through the natural continuation of their research, it was discovered that the mechanical insertion of the needle into the muscular tissue was as effective as a needle that applied medication. This evolution of trigger point dry needling research has provided an alternative to injected medication for pain relief. Research demonstrates that the insertion of the needle alone is sufficient enough to cause a therapeutic benefit via pain reduction or an abatement in abnormal muscular tone. Dry needling has gained popularity steadily since these discoveries, particularly with a resurged interest by healthcare professionals in the 2000s. It was strengthened by the mapping of pain patterns associated with different trigger points, and their interactions or influences on myofascial pain syndromes.
What conditions can it treat?
Conditions that benefit include:
- Ankle pain
- Elbow pain
- Hip pain
- Knee pain
- Shoulder pain
- Rotator cuff disorders
- Spinal pain including:
- Cervical pain
- Thoracic pain
- Lumbar pain
- Postural dysfunction
- Plantar fasciitis
- And other myofascial/muscle injuries
For further information regarding Trigger Point Dry Needling and to find out if this treatment is appropriate for you, please reach out to one of our physical therapists who will be happy to discuss this option with you.
- Segura-Orti E, Prades-Vergara S, Manzaneda-Pina L, Valero-Martinez R, Polo-Traverso J. Trigger point dry needling versus strain-counter strain technique for upper trapezius myofascial trigger points: A randomized controlled trial. Acupuncture in Medicine. 2016;34(3):171. https://search.proquest.com/scholarly-journals/trigger-point-dry-needling-versus-strain/docview/1793871810/se-2?accountid=41004. doi: http://dx.doi.org/10.1136/acupmed-2015-010868.
- Espejo-Antúnez L, Jaime Fernández-Huertas Tejeda, Albornoz-Cabello M, et al. Dry needling in the management of myofascial trigger points: A systematic review of randomized controlled trials. Complement Ther Med. 2017;33:46-57. https://search.proquest.com/scholarly-journals/dry-needling-management-myofascial-trigger-points/docview/1922855935/se-2?accountid=41004. doi: http://dx.doi.org/10.1016/j.ctim.2017.06.003.
- History of Dry Needling | Integrative Dry Needling Institute
- Acupuncture | Johns Hopkins Medicine

